Authored by Dr. Mary James, ND
You may be surprised when I tell you irritable bowel syndrome, or IBS, is extremely common among women. IBS can completely rule your life because you feel you have to plan your days and nights so you can always be close to a bathroom. IBS is poorly understood by many general practitioners who may offer medicines to quell the symptoms but not solve the issue at its source.

If you’ve been told that your digestive problems are all in your head, you should know that science shows that IBS stems from more than just our thoughts or from daily stress. While there is a mind-body connection to IBS, there are many other causes and also several natural approaches to relieving this miserable issue.
So you don’t have to focus your life around irritable bowel syndrome anymore. You can resolve the root source of your IBS and find relief for your digestive symptoms at the same time.
What is irritable bowel syndrome?
As a syndrome, IBS has a wide variety of symptoms in addition to bowel irritation. Scientists haven’t found physiological evidence of disease in the bowel, so a clear-cut definition has yet to be developed — and there isn’t a single test to diagnose it. Because of this, the functional medicine model is the most useful approach for treating it.
The following symptoms are frequently associated with IBS:
- Constipation
- Pain with bowel movements
- Painless diarrhea
- Alternating constipation and diarrhea
- Flatulence
- Nausea
- Vomiting
- Headaches
- Loss of appetite
- Early satiety
- Anxiety
- Depression
- Poor nutrient absorption
- Bloating
Some scientists think that IBS might exist on a spectrum together with inflammatory bowel disease (IBD). IBD includes ulcerative colitis as well as Crohn’s disease, and can cause visible changes to the intestines, which can become inflamed to the point where they are red and swollen. Some studies are aimed at pinpointing any molecular and structural changes within the bowels of various IBS patients, but there are still no definitive answers.
For conventional medicine, there are at least 4 main types of IBS to choose from:
- Diarrhea predominant IBS (IBS-D)
- Constipation predominant IBS (IBS-C)
- IBS with alternating stool patterns (IBS-A)
- Post-infectious IBS (IBS-PI)
The IBS subgroups keep changing so it’s no wonder women and doctors are confused about how to deal with IBS.
What causes irritable bowel syndrome?
While conventional practitioners do their best to address IBS symptoms, we believe that true healing of functional bowel disease can take place only when you treat the root causes. There is wide overlap between the causes and symptoms seen in IBS and other problems, such as yeast overgrowth, endometriosis, food sensitivities and more.
These can cause, influence, or exacerbate IBS, and they also lead to frequent misdiagnosis. For example, celiac can be overlooked when an IBS diagnosis is handed down, but it’s worth investigating before you rule out celiac as a cause of your symptoms.
The real solution as we see it is to address all IBS factors one by one so you can experience real results.
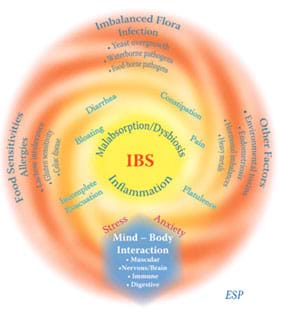
Causes and symptoms of irritable bowel syndrome
© 2008 Women’s Health Network
Major triggers for irritable bowel syndrome include:
Imbalanced gut flora
The bacteria that populate your gut are important not just to digestion, but to every aspect of your health. When you take an antibiotic, especially if it’s repeatedly, it can wipe out both kinds of bacteria — good and bad. If the friendly bacteria that help digest your food and protect the gut lining become imbalanced, then it compromises your digestive and immune function and can lead to IBS. Certain steroid medications and, overgrowth of yeast such as Candida in the intestines can lead to or worsen IBS.
GI infection
Research clearly shows a much higher incidence of IBS when you’ve had a GI infection. Some women develop IBS when they’ve had food poisoning or other intestinal parasites. Once you know about these pathogens, most can be easily treated with herbs or antibiotics.
Food sensitivities/intolerances
Many women with IBS also have unidentified food sensitivities or intolerances. Common culprits include foods such as wheat, gluten, dairy, corn, sugar, chocolate, coffee, tea and citrus fruits. Although food sensitivities and allergies can be complex and change over time, if you can identify and eliminate the problematic foods, your gut will quiet down and the symptoms of IBS often disappear.
Hormonal imbalance
Lots of women notice that their IBS symptoms are worst just before their periods. This may have to do with hormonal fluctuation in the second half of the cycle: estrogen is lower for several days and progesterone is relatively high at the end of the cycle, then drops off suddenly just before your period. Progesterone in general slows gut motility, and lower-than-normal estrogen has been identified in women with IBS.
Stress and anxiety
Of course, stress and anxiety can affect the body in many ways, including digestively. They change the autonomic nervous system — the system of nerves that make up the sympathetic (“fight or flight”) as well as parasympathetic (“rest and digest”) nervous systems. When you have IBS, the brain sends a message to decrease digestion and increase motility of the colon, resulting in the rapid passage of incompletely digested stool.
If you don’t pin down your IBS trigger from these, then there are many other disease processes that can lead to IBS-like symptoms and these should be ruled out by your practitioner. For example, endometriosis, ovarian and colon cancer, and inflammatory bowel disease can often cause bloating and other symptoms that resemble IBS, which can lead to a misdiagnosis.

The gut-brain connection — a piece of the IBS picture
It’s no surprise that when you have worries on your mind it can affect what happens in your gut. Most women know what it feels like to get butterflies before an important event, or to run to the bathroom before a test or even getting on a plane. There is another nervous system in your gut known as the enteric nervous system and we don’t know exactly how it affects irritable bowel syndrome.
Serotonin, the neurotransmitter associated with mood as well as brain function, is mostly manufactured in the gut. Its main role there is to stimulate intestinal movement and contraction as well as help with mucus secretion. Eating lots of simple carbs can cause a spike in serotonin levels which can trigger an episode of IBS, especially if you have issues with stress, a lack of digestive enzymes, flora imbalance, or other problems.
The nervous system is divided into the central nervous system (the brain and spinal cord) as well as the peripheral nervous system (all the other nerves in the body) and is controlled by the central nervous system. But the enteric nervous system (part of the peripheral nervous system) doesn’t always follow commands from the brain and spinal cord, and it doesn’t always send input back to the brain as the rest of the peripheral nervous system does.
The enteric nervous system can keep the gut working without input from the brain so it’s often called “the second brain.” This could then imply that IBS has nothing to do with the brain at all. But we do know that it takes a combination of healing the gut and the mind to heal IBS, so there is likely some key connection.
Relieve IBS symptoms by developing a healthy gut
When you want an individual’s whole health picture, the digestive system is a good place to start. But here in the West, we don’t always connect what’s happening in our bowels to overall health.
While some conventional practitioners consider it okay to have one bowel movement a week (!),a healthy digestive system should have a bowel movement once or twice a day.

Solving irritable bowel syndrome takes time because it involves some investigation and trial and error. Each woman heals differently, particularly when it comes to the gut, and the solution should be tailored to her unique physiology and situation.
If you have IBS here are the top options to try for relief:
Add a probiotic
Research shows that healthy probiotic flora such as Acidophilus, bifidobacteria and Saccharomyces boulardii may alleviate some cases of IBS. So, try a good probiotic and see if it relieves your irritable bowel. If you don’t get good results within two weeks, try another type of probiotic. Probiotics can also be found in fermented foods like yogurt, kefir and miso. Probiotic benefits include better digestion as well as improved immunity.
Experiment with food allergy testing or an elimination diet
If you have specific foods that trigger symptoms like gluten and lactose, eliminating them from your diet, at least temporarily, can help you feel much better. If you do decide on an elimination diet, then take a look at our Digestive Health Protocol. This kind of eating can be a little hard to manage but the results can make a world of difference.
Get a stool analysis
If your symptoms are not getting any better, then talk with your healthcare provider about getting a digestive stool analysis with comprehensive parasitology. This may provide answers about issues such as malabsorption, pH imbalance, parasites and yeast overgrowth. If your provider can’t help, then you can work with a lab on your own (see our testing options for labs). Treating parasites or also an abundance of yeast can dramatically reduce your IBS symptoms. A good functional medicine practitioner may recommend a protocol of functional foods and digestive enzymes to reverse inflammation in the bowel and related problems further up the digestive tract.
Make stress relief a real priority
No surprisingly, stress is the IBS trigger that can be the most difficult to resolve. If you’re in a longtime habit of feeling stressed and anxious, it’s hard to just change, especially if your stress grew out of worry and fear of your IBS symptoms. Women with IBS should be gentle to their digestion so introduce vitamin supplements slowly. Also, remember that what you think and feel has a deep impact on your body. Experiment with stress-relief techniques such as meditation, yoga, deep breathing and massage.
Take a good quality multivitamin
If your digestive process is compromised, then there’s no way you’re getting the micronutrients your body needs every day. So shore up your nutrition with a high quality multivitamin-mineral complex. Women with IBS should be gentle to the digestion so introduce vitamin supplements slowly.
Eat plenty of fiber
The bacteria in your gut need dietary fiber to do their jobs and they also use it to feed the cells in your colon. Choose fresh whole foods with lots of fiber such as vegetables, fruits and whole grains.
Try natural herbs
Herbs such as deglycyrrhizinated licorice root (DGL), enteric-coated peppermint, slippery elm bark, ginger, marshmallow, Swedish bitters and fennel seed can all help calm the symptoms of IBS with few side effects. Do some research yourself then consult with a qualified practitioner, for best results.
Reduce your IBS symptoms — it doesn’t have to be this way
Finally, IBS is not a simple disorder to treat. But the best way to begin the healing process is by understanding that your personal symptoms most likely have their own solutions. Then you can find your path to healthy, happy bowel function — naturally. And give us a call when you need a little help.
1 National Women’s Health Information Center, US Department of Health and Human Services. Irritable bowel syndrome. URL: https://www.4women.gov/FAQ/ibs.htm (accessed 03.06.2008).
2 Kennedy, T., et al. 2005. Cognitive behavioral therapy in addition to antispasmodic treatment for irritable bowel syndrome in primary care: Randomised controlled trial. BMJ, 331 (7514), 435. URL: https://www.bmj.com/cgi/content/full/331/7514/435 (accessed 03.06.2008).
3 Manning, A., et al. 1978. Towards positive diagnosis of the irritable bowel. Brit. Med. J., 2 (6138), 654–655. URL (full text): https://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pubmed&pubmedid=698649 (accessed 03.06.2008).
Watson, B., & Smith, L. 2004. Gut Solutions: Natural Solutions to Your Digestive Problems, p. 139. Clearwater, FL: Renew Life Press.
4 Bercik, P., et al. 2005. Is irritable bowel syndrome a low-grade inflammatory bowel disease? Gastroenterol. Clin. North Am., 34 (2), 235–245, vi–vii. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/15862932 (accessed 02.28.2008).
5 Familydoctor.org editorial staff. 2006. Inflammatory bowel disease. What is inflammatory bowel disease. URL: https://familydoctor.org/online/famdocen/home/common/digestive/disorders/252.html (accessed 03.06.2008).
6 Talley, N. 2006. A unifying hypothesis for the functional gastrointestinal disorders: Really multiple disease or one irritable gut? Rev. Gastroenterol. Disord., 6 (2) ,72–78. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/16699476 (accessed 03.06.2008).
7 Gershon, M. 1999. The Second Brain, p. 187. NY: Harper Collins.
8 Natural Standard. 2008. Irritable bowel syndrome (IBS). URL: www.naturalstandard.com/monographs/conditions/condition-irritablebowelsyndrome (accessed 02.20.2008).
9 Chang. L. 2006. From Rome to Los Angeles — The Rome III Criteria for the gunctional GI disorders. URL (PDF): https://www.romecriteria.org/pdfs/RomeCritieraLaunch.pdf (accessed 03.06.2008).
10 Enck, P., & Martens, U. 2008. The next consensus for the irritable bowel syndrome has to be interdisciplinary. Z. Gastroenterol., 46 (2), 211–215. URL: https://www.ncbi.nlm.nih.gov/pubmed/18253901 (accessed 03.06.2008).
11 Santelmann, H., & Howard, J. 2005. Yeast metabolic products, yeast antigens and yeasts as possible triggers for irritable bowel syndrome. Eur. J. Gastroenterol. Hepatol., 17 (1), 21–26. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/15647635 (accessed 03.06.2008).
12 Lipski, E. 2004. Digestive Wellness. 3rd ed., p. 256. NY: McGraw Hill.
13 Ford, A., et al. 2009. Yield of diagnostic tests for celiac disease in individuals with symptoms suggestive of irritable bowel syndrome. Arch. Intern. Med., 169 (7), 651–658. URL (abstract): https://www.ncbi.nlm.nih.gov/entrez/19364994 (accessed 07.06.2009).
“The prevalence of biopsy-proven celiac disease in individuals who met diagnostic criteria for IBS was fourfold higher than for controls without IBS,” says Ford, who works at McMaster University, Canada. “Celiac disease should therefore be sought out and excluded before labeling individuals as suffering from IBS,” he continues.
“Future research should examine whether the increased prevalence of celiac disease in IBS is constant across the various subgroups of patients with IBS,” concludes Ford.
14 Parry, S., et al. 2003. Does bacterial gastroenteritis predispose people to functional gastrointestinal disorders? A prospective, community-based, case-control study. Am. J. Gastroenterol., 98 (9), 1970–1975. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/14499773 (accessed 03.06.2007).
15 Ruigómez, A., et al. 2007. Risk of irritable bowel syndrome after an episode of bacterial gastroenteritis in general practice: Influence of comorbidities. Clin. Gastroenterol. Hepatol., 5 (4), 465–469. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/17445753 (accessed 02.28.2008).
16 Mearin, F., et al. 2005. Dyspepsia and irritable bowel syndrome after a Salmonella gastroenteritis outbreak: One-year follow-up cohort study. Gastroenterology, 129 (1), 98–104. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/16012939 (accessed 02.28.2008).
17 Marshall, J., et al. 2006. Incidence and epidemiology of irritable bowel syndrome after a large waterborne outbreak of bacterial dysentery. Gastroenterol., 131 (2), 445–450, quiz 660. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/16890598 (accessed 02.28.2008).
18 Marshall, J., et al. Postinfectious irritable bowel syndrome after a food-borne outbreak of acute gastroenteritis attributed to a viral pathogen. Clin. Gastroenterol. Hepatol., 5 (4), 457–460. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/17289440 (accessed 02.28.2008).
19 Snider Sachs, J. 2005. Are antibiotics killing us? Discover, 26 (10). URL (full text): https://discovermagazine.com/2005/nov/are-antibiotics-killing (accessed 03.06.2007).
20 Lipski, E. 2004. Digestive Wellness. 3rd ed., 254. NY: McGraw Hill.
21 Cui, N. et al. 2006. [Association of peripheral blood estradiol, progesterone, and testosterone levels with irritable bowel syndrome.] Nan Fang Yi Ke Da Xue Xue Bao, 26 (3), 367–368. URL (full-text PDF, in Chinese): https://www.jfmmu.com/pdf2/200603/200603367.pdf (accessed 03.06.2008).
The authors state in the abstract:
“In the female patients, blood estradiol level was significantly lower than that of the control group (P<0.05), whereas blood progesterone and testosterone levels had no significant differences between the two groups (P>0.05)…. CONCLUSION: Peripheral blood … estradiol level[s] in female patients are lower than those of healthy subjects, suggesting that IBS might be associated with blood sex hormone disorder.”
22 Lagus, J., et al. 2007. The central role of gastrointestinal-specific anxiety in irritable bowel syndrome: Further validation of the Visceral Sensitivity Index. Psychosom. Med., 69 (1), 89–98. URL (abstract): https://www.psychosomaticmedicine.org/cgi/content/abstract/69/1/89 (accessed 02.28.2008).
23 Lumpkin, M. 2007. 21st century endocrinology: Thyroid and adrenal as sentinel organs. IFM Conference CD #6. Tucson, AZ, 05/23–05/26/2007.
24 Lipski, E. 2004. Digestive Wellness. 3rd ed., 28. NY: McGraw Hill.
25 Gershon, M. 1999.The Second Brain, p. 17. NY: Harper Collins.
26 Berman, S., et al. 2008. Reduced brainstem inhibition during anticipated pelvic visceral pain correlates with enhanced brain response to the visceral stimulus in women with irritable bowel syndrome. J. Neurosci., 28 (2), 349–359. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/18184777 (accessed 03.06.2008).
Chang, L. 2005. Brain responses to visceral and somatic stimuli in irritable bowel syndrome: A central nervous system disorder? Gastroenterol. Clin. North Am., 34 (2), 271–279. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/15862935 (accessed 03.06.2008).
27 Lipski, E. Digestive Wellness. 3rd ed., p. 256. NY: McGraw Hill.
28 Kajander, K., et al. 2008. Clinical trial: Multispecies probiotic supplementation alleviates the symptoms of irritable bowel syndrome and stabilizes intestinal microbiota. Aliment. Pharmacol. Ther. 27 (1), 48–57. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/17919270 (accessed 03.03.2008).
Kajander, K., & Korpela, R. Clinical studies on alleviating the symptoms of irritable bowel syndrome. Asia Pac. J. Clin. Nutr., 15 (4), 576–580. URL: https://www.ncbi.nlm.nih.gov/pubmed/17077079 (accessed 03.03.2008).
Whorwell, P., et al. 2006. Efficacy of an encapsulated probiotic Bifidobacterium infantis 35624 in women with irritable bowel syndrome. Am. J. Gastroenterol., 101 (7), 1581–1590. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/16863564 (accessed 03.03.2008).
29 Lackner, J., et al. 2007. How does cognitive behavior therapy for irritable bowel syndrome work? A mediational analysis of a randomized clinical trial. Gastroenterology, 13 (2), 433–444. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/17681164 (accessed 03.06.2008).
Kennedy, T., et al. 2006. Cognitive behavioural therapy in addition to antispasmodic therapy for irritable bowel syndrome in primary care: Randomised controlled trial. Health Technol. Assess., 10 (19), iii–iv, ix–x, 1–67. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/16729918 (accessed 03.06.2008).
30 Lipski, E. 1999. Digestive Wellness, 32. NY: McGraw–Hill.










