Authored by Dr. Mary James, ND
Perimenopause is the natural transition between healthy, reproductive function and menopause, or 12 consecutive months without a menstrual period.

Perimenopause can begin anywhere between your mid-30s and 50s, but the median age is 47.5 years, with menopause occurring at an average age of 52. As a key stage in a woman’s life, perimenopause is a biological progression, not an actual event. Still, you can’t know ahead of time how long it will last.
Perimenopause is a big deal for many women because their reproductive hormones start to fluctuate. As estrogen, progesterone and testosterone shift and decrease, they fall out of balance with each other. This imbalance can lead to a surge of symptoms that may last for years.
To know if you’re in perimenopause, investigate your symptoms for clues. If your symptoms are new, suddenly worse than before, or have no clear pattern, you’re probably experiencing the hormonal imbalance of perimenopause.
What are the symptoms of perimenopause?
Symptoms are a solid confirmation that your perimenopause transition has begun. Hormone-related perimenopause symptoms include:
- Irritability
Irritability is the top complaint among perimenopausal women. It’s triggered by abrupt and extreme hormone fluctuations that affect key neurotransmitter systems in the brain. - Anxiety
Anxious feelings rooted in hormonal imbalance may feel manageable at first, but can grow out of control as the process of perimenopause proceeds. - Weight gain
Incredibly common and extremely discouraging, perimenopausal weight changes are usually made worse by stress and its cascade of effects. - Adult acne
Skin changes, like dryness and wrinkles, are expected as you get older, but many women are surprised to experience hormonal acne, pimples and breakouts, especially on the chest and upper back. - Depressed feelings and moodiness
When a woman hits perimenopause, her moods can be destabilized by disruptions in estrogen and progesterone, which compounds worry and sadness about natural life changes. - Irregular periods
Menstrual changes are often the first sign of perimenopause, with periods becoming longer, shorter, lighter or heavier, depending on physiology and other factors. - Joint pain
Since estrogen has an anti-inflammatory effect, when it begins its natural midlife decline, you may notice inflammation symptoms, like joint pain in knees, elbows, hands, feet, etc. - Menstrual migraines
Migraines often have a hormonal component, so these miserable, long-lasting menstrual migraine headaches may be triggered as estrogen falls out of balance to progesterone. - Memory issues or fuzzy thinking
As estrogen and progesterone levels jump around during perimenopause, memory issues and cognitive concerns often emerge. - Sleep problems
Insomnia is a huge problem for women in perimenopause, often linked to adrenal stress, and exacerbated by imbalanced reproductive hormones. - Hot flashes and night sweats
As the signature symptoms of perimenopause, hot flashes are fueled by intense hormonal ups and downs, with some women having only a handful, and others experiencing 20-30, or more, a day. - Vaginal dryness
Vaginal changes at midlife include dryness, atrophy and itching, reducing libido and causing discomfort, or even pain, during sex. - Low sex drive
Changes in reproductive hormone levels, and how they’re regulated by the body, can cause sex drive to plunge.
What causes all these perimenopause symptoms?
While changing hormones are the cause of midlife symptoms, it’s not true that perimenopause means a gradual but steady decline in estrogen. In fact, estrogen levels can climb higher in perimenopause than they’ve been for years — sometimes resulting in dramatic menstrual changes.
Another misconception is that all symptoms are caused by decreased estrogen. Instead, it is hormonal fluctuations that cause symptoms to develop. When fluctuations are extreme or occur too quickly, your body cannot manage them, and things begin to go off course in your body.
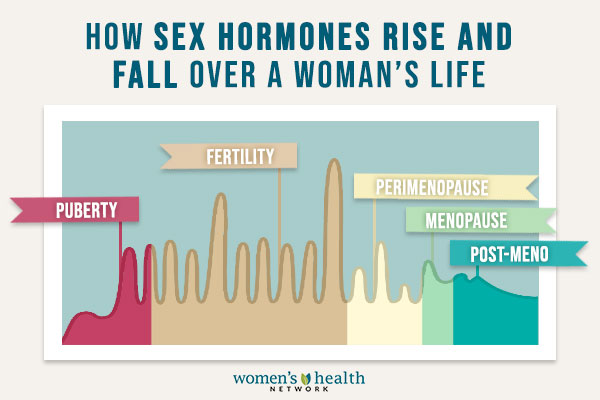
Fluctuations in other hormones also have a big effect during perimenopause. Follicle stimulating hormone (FSH), luteinizing hormone (LH), progesterone, testosterone and DHEA are all shifting too, which can worsen perimenopause symptoms.
What happens to your hormones as you enter perimenopause?
Sex hormone levels and the menstrual cycle are regulated by the constant three-way feedback of the hypothalamus, the pituitary gland and the ovaries. For this hypothalamic-pituitary-ovarian axis to function properly, each area must be sensitive enough to respond to incoming signals from the others.
But the number of ovary follicles (sacs that each contain an immature egg) declines with age, making them less able to be responsive to incoming messages.
To compensate, the hypothalamus amps up its signaling, including making changes to FSH and LH until it’s almost as if they’re yelling louder to get attention. In perimenopause, the ovaries may not answer the call at all, or they may be hyper-responsive to the loud FSH signal and make estrogen levels spike.
Your body is naturally equipped to deal with changing levels of hormones. But life happens, and certain factors can have severe effects on your hormones, such as:
- poor diet
- chronic stress
- sleep problems
- not enough exercise
- exposure to environmental toxins
Even issues that start off small when you’re young can push your hormones out of sync as you hit perimenopause. Eventually, your body’s gentle coping methods are not enough to compensate. During times of life with the most dramatic changes — such as perimenopause — your hormones can cause intense symptoms. That’s why it’s crucially important to take steps to provide support for your body so it can restore hormonal balance.
What makes you more likely to have horrible perimenopause symptoms?
Having hormonal symptoms earlier in life makes you more prone to having them in perimenopause too. Having had PMS makes you twice as likely to have perimenopause symptoms. If depressed feelings are one of your PMS symptoms, or if you’ve had them after childbirth, or while using birth control pills, you may experience depression in perimenopause too.

Chronic stress and emotional strains, like financial worries or caring for aging parents, can add extra weight to the burdens you carry in perimenopause. Some of these factors are impossible to change but you can do something about others, and stress should be at the top of the list.
Chronic stress seriously magnifies the effects of changing sex hormones and neurotransmitter levels in perimenopause and menopause. That’s because your body uses the same basic building blocks to make both adrenal stress hormones (cortisol) and sex hormones. But when you are buried under chronic stress, your body has to choose so it prioritizes non-stop production of cortisol. Just when you need it the most, sex hormone production is forced to take a backseat.
But you can change that. Stress management and adrenal support can help redirect your body’s resources away from the fight-or-flight response, and turn it toward balancing reproductive hormones. In our fast-paced, device-centered, eat-and-run world, younger and younger women are now experiencing perimenopausal-type symptoms.
How can you relieve perimenopause symptoms and feel better?
The signs and symptoms are much the same for both perimenopause and menopause. For the most effective, longest lasting perimenopause symptom relief, consider a commonsense approach that includes the following:
1. Eat a healthy diet.
If you haven’t been taking a good multivitamin, give it a try for a couple of months to use nutrition to help heal your hormonal pathways. A good nutritional foundation can help ensure your body has the raw materials it needs to complement the food you eat. See if you can cut back on sugar, carbs and wheat.
Eat plenty of vegetables and add in some healthy fats (olive oil, avocado, omega-3s), small amounts of lean protein (poultry, fish, plant-based options), and a few whole grains (oats, quinoa, buckwheat). Go slowly if you have to, but keep nudging yourself to eat healthier. Your hormonal health is guaranteed to improve as you ditch sweets and bread items.

2. Find enjoyable exercise.
If you don’t like exercise, just start walking a few times a week and build up your distance as you go. Physical movement is one of the most important ways to defuse perimenopause symptoms, and it releases stress and tension very effectively. Other helpful practices for relieving stress include slow, deep breathing through your nose (it’s not any more complicated than it sounds) and meditation (it takes some practice but is worth every bit of effort).
3. Restore hormonal imbalance with targeted herbs and nutrients.
Using phytotherapy, or medicinal herbs, is the easiest part of recovering hormonal balance for perimenopause symptom relief. Phytotherapy mimics your body’s hormonal actions at a molecular level to help balance out the highs and lows. These types of herbal supplements for menopause also interact with your body’s tissues to facilitate natural hormone regulation.
4. Pay close attention to your emotional health.
The emotional piece is one of the hardest for women in perimenopause. You may even feel as if you’ve spent a lifetime entrenched in the same unhealthy patterns. But you can change this with time, patience and a little help from your friends (or a great therapist for the big stuff). Nothing is more liberating than letting go of emotional burdens that have been weighing down your spirit.
5. Carve out time for rest and relaxation.
If your days are crammed full of tasks, with lots of extra activities packed in at night, you’ve got a lot going on. Over time, this go-go pattern takes a physical toll and drains you mentally and emotionally. Perimenopause is the right time to force yourself to shift gears for your health, and hormonal balance. Block out at least a half hour a day to wind down, read, nap or just do nothing.

Let yourself feel good in perimenopause
If you don’t understand the changes happening in your body, perimenopause can be miserable, and there are so many confusing menopause myths out there. Perimenopause is a natural transition, but symptoms do not have to be part of the equation. If you can accept, and even embrace, where you are on the reproductive timeline, you can find powerful relief for both your physical and emotional symptoms.
I encourage you not to let your symptoms define you during this stage of life. Perimenopause is a real opportunity to live your life on your own terms so you can feel healthier and happier than ever.
References and further reading
Nanette Santoro, MD. Perimenopause: From Research to Practice. J Womens Health (Larchmt). 2016 Apr 1; 25(4): 332–339. Accessed 11.19.18.
Clayton AH, Ninan PT. Depression or menopause? Presentation and management of major depressive disorder in perimenopausal and postmenopausal women. Prim Care Companion J Clin Psychiatry. 2010;12(1):PCC.08r00747.
Clayton AH, Ninan PT. Depression or menopause? Presentation and management of major depressive disorder in perimenopausal and postmenopausal women. Prim Care Companion J Clin Psychiatry. 2010;12(1):PCC.08r00747.
Burger HG, Hale GE, Robertson DM, Dennerstein L. A review of hormonal changes during the menopausal transition: focus on findings from the Melbourne Women’s Midlife Health Project. Hum Reprod Update. 2007 Nov-Dec;13(6):559-565.
Woods NF, Mitchell ES. Symptoms during the perimenopause: prevalence, severity, trajectory, and significance in women’s lives. Am J Med. 2005 Dec 19;118 Suppl 12B:14-24.
Burger HG, Hale GE, Robertson DM, Dennerstein L. A review of hormonal changes during the menopausal transition: focus on findings from the Melbourne Women’s Midlife Health Project. Hum Reprod Update. 2007 Nov-Dec;13(6):559-565.
Freeman EW, Sammel MD, Rinaudo PJ, Sheng L. Premenstrual syndrome as a predictor of menopausal symptoms. Obstet Gynecol. 2004 May;103(5 Pt 1):960-966.
Stewart DE, Boydell KM. Psychologic distress during menopause: associations across the reproductive life cycle. Int J Psychiatry Med. 1993;23(2):157-162.
Freeman EW, Sammel MD, Lin H, Nelson DB. Associations of hormones and menopausal status with depressed mood in women with no history of depression. Arch Gen Psychiatry. 2006 Apr;63(4):375-382.
Woods NF, Mitchell ES. Symptoms during the perimenopause: prevalence, severity, trajectory, and significance in women’s lives. Am J Med. 2005 Dec 19;118 Suppl 12B:14-2










