Today experts consider the IUD — or intrauterine device — one of the most effective forms of birth control, with only abstinence ranking higher. And while a lot of women in their 40’s and 50’s grew up hearing horror stories about safety issues during the early days of IUDs, these devices actually cause very few or even no side effects for most women.
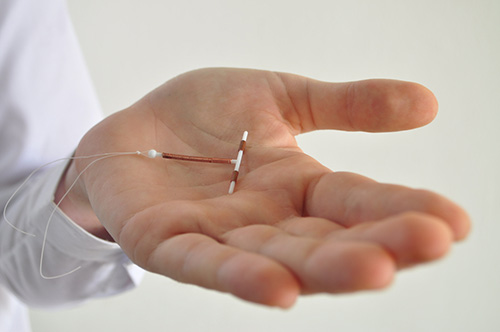
But the old reputation persists, even among some doctors and healthcare providers.
There were two main problems with the old IUDs. First, the design of an early device called the Dalkon Shield was flawed, which led to pelvic injuries and higher rates of pelvic inflammatory disease, or PID. Second, other, much safer IUDs were then blamed for cases of PID and women — and their doctors — did not want to use them.
Research suggests that the risk of PID associated with IUD use is mostly limited to the first 3 weeks after insertion — especially high if a woman has a preexisting but unknown chlamydia infection. Fortunately, it’s uncommon after that.
So be sure to share any concerns with your healthcare provider — both before and after IUD insertion, and get routine follow-up.
With the exception of condoms, contraceptives do not protect against sexually transmitted diseases. STDs are a significant and growing health risk to women of all ages, including menopausal women, either through partner infidelities or unprotected sexual encounters.
Learn how to minimize your risks from our article on safe sex in midlife.
The IUD problems of 30–40 years ago were in IUDs that had a different design. And that doctors probably gave to women with multiple partners — a time when HIV and AIDs were unheard of. At that time, medicine did not have effective testing for chlamydia — the infection that is the cause of most PID and infertility.
Intrauterine systems
IUDs today have a much better design, following years of research and improvement. Some manufacturers now refer to their IUD product as intra-uterine system, or IUS. New technologies have made them a great option for many women, particularly perimenopausal women and mothers who don’t want more children. The ideal candidate for an IUD is an infection-free woman in a monogamous relationship, who has had at least one pregnancy (for ease of insertion), and whose uterus is free of fibroids.
Options include the 10-year copper ParaGard IUD which is hormone-free, and the 5-year Mirena IUS, which releases small amounts of hormones into the uterus. Women with a history of blood clots can use the T-shaped copper device. Mirena releases a synthetic progestin hormone internally and works well when a woman has heavy bleeding.
The NuvaRing is a 21-day vaginal insert that conveniently delivers a consistent, very low dose of birth control hormones. It’s different from the birth control pill which must go through your digestive tract and involve the liver. The low dose and steady release of this product make it a good alternative to pills for women who have symptoms like hormonal headaches. Another plus for some women is that their vaginal moisture is maintained better with the NuvaRing than with oral contraceptives.
An intrauterine system is an excellent option if you enjoy the sexual spontaneity that you get with the Pill. A woman can almost forget about an IUS or IUD once it’s in place, until it’s time to remove it. There are a number of additional considerations that may or may not apply to you. So if you’re interested in an IUS or IUD, then talk to your practitioner. And if you do choose an IUD, be sure to keep your follow-up visits.
Other non-hormonal birth control options for women
Barrier methods like condoms, the diaphragm, and the new Today Sponge — yes, it’s back — are relatively reliable birth control methods that don’t rely on hormones. The Sponge has been available in the USA and FDA-approved since April 2005.
For women who are finished having children and for those who don’t want children, permanent surgical options include tubal ligation (having your tubes “tied”), or for the male partner, vasectomy.
The choice is yours
With so many factors to consider when choosing a birth control method, women need to find the specific contraceptive options that will work well for them. Each woman has unique needs to consider, and those can change over the course of her reproductive years. She may start out on the Pill but then move to an IUD or an IUS after she’s had a child.
1 Grimes, D. 1992. The intrauterine device, pelvic inflammatory disease, and infertility: the confusion between hypothesis and knowledge. Fertil Steril., 58 (4), 670–673. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/1426307 (accessed 05.06.2011).
2 [No authors listed.] 2009. Intrauterine devices: an effective alternative to oral hormonal contraception. Prescrire Int., 18 (101), 125–130. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/19637436 (accessed 05.06.2011).
3 Backman T. 2004. Benefit-risk assessment of the levonorgestrel intrauterine system in contraception. Drug Saf., 27 (15), 1185–1204. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/15588115 (accessed 05.06.2011).
4 [No authors listed.] 2009.
References on the IUD and pelvic inflammatory disease
1 [No authors listed.] 2009. Intrauterine devices: An effective alternative to oral hormonal contraception. Prescrire Int., 18 (101), 125–130. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/19637436 (accessed 05.06.2011).
Grimes, D. 2000. Intrauterine device and upper-genital-tract infection. Lancet, 356, 1013–1019. URL (abstract): https://www.ncbi.nlm.nih.gov/pubmed/11041414 (accessed 05.06.2011).










