A hysterectomy is a surgical procedure to remove a woman’s uterus. “Do I need a hysterectomy? What are my alternatives?” These are common questions for women struggling with heavy bleeding or fibroids, or one of the other problems that may lead to hysterectomy.

Women may feel that surgery is the only choice but in a lot of cases, there are other options. Many women have great success with alternatives to hysterectomy and even when surgery is required, new techniques are often much less invasive than they used to be.
It’s likely that you already know women who’ve had hysterectomies — about a third of American women have one by age 60. For some it is a relatively easy experience, but for others the aftermath of surgical menopause is made worse by severe hormonal symptoms and eventual dependence on hormone replacement therapy (HRT). Since hysterectomy is considered elective surgery for some women, they are sometimes unprepared for the debilitating after-effects.
If you are faced with this decision, you will want to weigh the benefits versus the risks of hysterectomy with your practitioner, in light of your own health history. The more you know, particularly about alternatives, new technology and procedures, the better equipped you’ll be to make the right choice.
Before you have a hysterectomy: understand the basics
The uterus, or womb, is a pelvic organ suspended by ligaments between the bladder and rectum and connected to the vagina with the cervix.
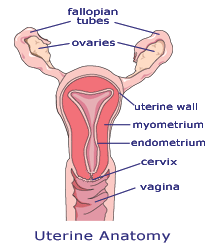
The fallopian tubes carry eggs from the ovaries to the uterus. The uterus can be positioned toward the front or back of the pelvis (anteverted or retroverted). The lining, or endometrium, of the uterus swells with each menstrual cycle — becoming engorged in preparation for the implantation of a fertilized egg. The body sheds this lining with a menstrual period if that doesn’t happen. If implantation does occur, the uterus expands for nine months to accommodate the fetus’s growth, then shrinks back to size after delivery and the process starts all over.
This process is orchestrated by the complex crosstalk between your sex hormones — mostly estrogen, progesterone and testosterone. Before menopause, your ovaries produce most of your body’s estrogen and progesterone. This is important to think about when considering a hysterectomy because of what may happen when any of those organs is removed.
If you have been struggling for years with heavy bleeding or painful fibroids, it may seem simpler to have all your reproductive organs removed. But we urge you to get more information first. That’s because we now know that often, total hysterectomy, including removal of the ovaries, leaves many women feeling wrecked due to loss of their natural ovarian hormones. So if you have a choice about having a hysterectomy, ensure that the most recent information and insight about hysterectomy are being applied to your case. Even if this is met with resistance by your doctor you should probably seek a second opinion prior to being scheduled for hysterectomy surgery.
The history of hysterectomy
The term hysteria (Latin for uterus) comes directly from the belief that the uterus could produce wild fits of fainting, crying and laughing. Hysteria was considered a form of mental instability. In Victorian times, if a woman’s temperament could not be “controlled,” it was common for her reproductive organs to be removed. Only within the last century have we recognized that the brain controls our emotions, and that taking out a woman’s reproductive organs often causes more problems than it solves.
Common reasons for elective hysterectomy
Hysterectomy is the second-most common major surgery performed on women in the United States. Each year, more than 600,000 women undergo hysterectomy with a conservative estimate that between 20–30% of them are medically unnecessary.
There are several reasons why women are advised to consider an elective hysterectomy. The most common are heavy bleeding, large fibroids, endometrial polyps, endometriosis, and other endometrium issues. Some women want a hystectomy to be more comfortable, or they have a prolapsed uterus, a condition in which the pelvic organs drop. But it’s different with more serious indications, including cancers of the uterus or ovaries. These conditions merit immediate surgery. In these relatively rare cases, a woman does not truly have a choice and hysterectomy is a life-saving solution, offering reassurance and peace of mind.
But most women may want to consider their options before scheduling surgery.
Heavy bleeding
Conventional medicine brands heavy bleeding as “dysfunctional uterine bleeding” because it’s assumed that the loss of blood is not healthy and serves no purpose for a woman. However, the body, as part of a natural process, is trying to do what it is supposed to: shed the uterine lining. And it’s also true sometimes that what is dysfunctional for one person may not be for another
Often, environmental and lifestyle factors affect our hormones and send the uterus mixed messages. These can, for example, lead to a state of estrogen dominance or cause the menstrual cycle to be out of sync, leading to overall hormonal imbalance. Tuning in and paying attention to what your body needs can restore balance naturally.
Even with the best efforts, it can take several months for a woman to restore balance. Heavy bleeding is miserable and uncomfortable, with the added nuisance of having to change pads or tampons frequently, wash extra bed sheets and limit and time activities around heavy flow. When women in this situation ask for a hysterectomy, most doctors in America will say yes. But usually, surgery shouldn’t be the first or even the second option for heavy bleeding. No matter what, bleeding eventually stops — when a woman goes through menopause.
Heavy bleeding often occurs around perimenopause and in many cases can be effectively addressed with many natural measures before pursuing surgery. In most cases, a woman with dysfunctional uterine bleeding can try surgical intervention such as “medical management” of dysfunctional bleeding before “surgical management.” This cautious approach is generally safe, as long as the lining of the uterus has been appropriately evaluated with an endometrial biopsy or D&C if necessary, and as long as the red blood count remains adequate.
Many women with heavy bleeding get excellent results by using high-dose bioidentical progesterone, as creams or oral tablets, along with other supportive supplements. Lifestyle and dietary changes that reduce stress and increase core nutrition are also highly effective.
Bleeding issues often reflect irregularities of the endometrium with symptoms strongly influenced by the monthly ebb and flow of estrogen as well as progesterone. These problems often respond well to a natural rebalancing of hormones through diet and lifestyle changes. You may want to try this before turning to surgical intervention partially because organ removal can lead to different problems.
Postmenopausal bleeding
Postmenopausal bleeding is different — any bleeding that occurs after menopause should be evaluated immediately by your healthcare provider. You may be referred for vaginal ultrasound so the endometrium within the uterus can be evaluated and measured. If the endometrial stripe is greater than a certain width, endometrial biopsy is recommended. Certain drugs, such as tamoxifen for breast cancer, can cause endometrial thickening.
Adenomyosis
Persistent heavy bleeding that doesn’t have an identifiable source such as fibroids, and that does not respond to medical management, is often a result of adenomyosis of the uterus (sometimes referred to as endometriosis interna). In this condition, which is sometimes mistaken for uterine fibroids, the glandular endometrial lining of the uterus invades the bulk of the uterine muscle wall.
While many women who have adenomyosis have no symptoms, it can cause the uterus to grow 2–3 times its normal size, accompanied by severe menstrual cramping. It can sometimes be identified by ultrasound, or more definitively by MRI, and confirmed by pathology after hysterectomy, though it’s technically categorized as a benign condition.
If you have exhausted all natural measures and still have persistent heavy bleeding, you may want to ask about adenomyosis as a potential diagnosis. Endometrial ablation is one alternative to hysterectomy now available, along with the Mirena IUD, and either may be considered in certain cases.
Fibroids
At least 40% percent of hysterectomies are for fibroids though fibroids are not technically part of the endometrium. No one knows exactly what causes them, but they are definitely an issue for many women. Their growth may be fueled by estrogen but we don’t know for sure yet.
At least one in five women over age 35 has fibroids. Many women think that having fibroids will eventually lead to having a hysterectomy but this isn’t necessarily true. Some doctors may recommend a hysterectomy for fibroids even when there is no bleeding or pain. Surgery is likely not needed in this scenario.
Many women deal successfully with their fibroids through diet, lifestyle and supplements — as well as acupuncture, if there is pain. See our fibroid article for more information on causes and natural treatment for fibroids.
Fibroids can cause bleeding and pain or discomfort, and can grow in some cases. A fibroid’s size is compared to the gestational age of a fetus — for example, a 5-month size fibroid — or to a piece of fruit (orange or melon-sized). Women can have multiple fibroids of various sizes and shapes, and some change very little over time, with many women unaware of them. A healthcare provider can often feel them during a pelvic exam and will order an ultrasound if warranted.
An ultrasound measures the fibroid and helps assess it. You may be referred for repeat ultrasounds to be sure the fibroids aren’t growing too large or too rapidly. Your doctor may also order a CT scan or an MRI if additional information is needed. Fibroids are very rarely cancerous and do not routinely need to be biopsied. But be aware that any kind of dysfunctional uterine bleeding usually mandates an endometrial biopsy to rule out potentially more threatening, co-existing issues.
Polyps
Uterine polyps or endometrial polyps are irregularities of the inner uterine lining, sort of like fleshy skin tags, only on the inside. Polyps can be a source of irregular bleeding but they are not usually cancerous. However, they can change over time.
Polyps of the uterine lining may be difficult to see on regular ultrasound, but a “sono-hyst” (sonohysterography) or saline-infused ultrasound may help visually define the nature of a polyp more accurately. Fragments suggestive of polyps can also be identified by endometrial biopsy.
Most endocervical polyps can be removed through the vagina, without affecting the uterus, but uterine-endometrial polyps are generally removed via the D&C with hysteroscopy method — slightly invasive but still less traumatic than a hysterectomy.
Endometriosis
Endometriosis is a condition that is generally more troublesome than truly health-threatening. Many women who have endometriosis don’t know they have it until they try to get pregnant. Endometriosis can cause fertility problems, but is even more notorious for causing irregular spotting, bleeding and pain. If you have severe endometriosis, the pain can be debilitating, especially around your period.
Acupuncture can be quite helpful for pain management. If fertility is an issue, you can try massage techniques such as integrative manual therapy (IMT) or Clear Passages therapy. Laparoscopy is often used in more severe cases for definitive diagnosis and treatment. See our article for more detailed information on natural treatments for endometriosis.
If your decision to have a hysterectomy is an elective one, take the time to fully research your choices and determine how you might be able to try a natural approach before you commit to surgery.
Different kinds of hysterectomy procedures
Many women of earlier generations didn’t know exactly what a hysterectomy entails. Today, there are several different types of hysterectomy, as well as additional techniques used to perform them. If you are considering hysterectomy, learn about the specifics of each kind and discuss them in advance with your practitioner.
Total hysterectomy
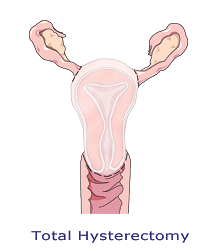
In a total hysterectomy, the entire uterus and cervix are removed and ovary status is officially referred to separately. Total hysterectomy (TAH) can be done abdominally with an incision typically made along the bikini line. In an emergency, a vertical incision is made through the abdominal wall from the belly button to the pubis. TAH can also be performed through the vagina, without a large incision through the belly.
The most sophisticated techniques use laparoscopy to assist the hysterectomy procedure. In laparoscopic hysterectomy, the organs are visualized and manipulated through a laparoscope, and the uterus is removed either through the vagina (laparoscopically-assisted vaginal hysterectomy, or LAVH) or through a small incision in the abdomen. The incisions are very small (~½”, beneath the belly button and on the lower pelvis/abdomen, beneath the bikini line).
This surgery lends itself to faster recovery, with far less disruption of the bowel and pelvic floor architecture. It is best performed by a laparoscopic specialist, as not all surgeons are skilled at this. The choice here depends on the reasons for doing the surgery, the patient’s anatomy, and the surgeon’s preference. If you have a preference, clearly communicate this to your surgeon.
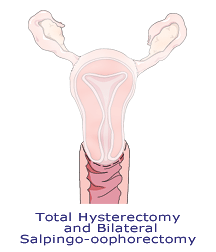
While doing a hysterectomy, a surgeon may also remove the ovaries and fallopian tubes with a bilateral salpingo-oophorectomy (BSO, or together with a total abdominal hysterectomy, TAH/BSO.) There are many considerations to make before consenting to this surgery, starting with the artificial onset of menopause due to loss of your natural sex hormones. Again, the decision depends on the individual nature of a woman’s condition and her doctor’s choices. If this is the option available to you, be assured that it is possible to regain hormonal balance with the help of some good support measures and a healthy lifestyle. You can talk it over with your doctor later if you need additional help.
Young women who must undergo a BSO usually should consider appropriate estrogen replacement for numerous health benefits.
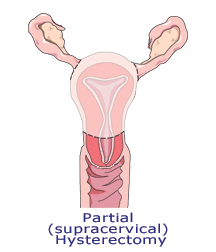
Partial hysterectomy
In a partial or subtotal — supracervical = above the cervix — hysterectomy, the ovaries and/or cervix are left intact. These procedures can be also performed abdominally, vaginally or laparoscopically. Unfortunately, many women aren’t told about these options and sometimes the cervix is removed automatically as a precaution against cervical cancer.
You should definitely talk this over with your doctor, and the surgeon performing your hysterectomy, if they’re different. Many women have seen that the benefits of retaining the cervix — more sexual enjoyment and sounder inner pelvic architecture — outweigh the relative risks. An intact cervix may actually benefit proper Pap smear technique so if you choose to keep your cervix, continue regular annual screenings and Pap tests.
Another option is a laproscopically-assisted supracervical (partial) hysterectomy (LASH, or LSH). This allows women to try to keep their ovaries (no BSO), if possible, but this is case-dependent. Try to find a doctor skilled in these newer techniques, many of whom specialize in endometriosis treatment.
We also recommend preparing yourself for surgery. You can sign up for a few sessions of acupuncture, and use Peggy Huddleston’s book and CD, Prepare for Surgery, Heal Faster to decrease your recovery time and possibly improve your outcome.
Alternatives to hysterectomy
If you have the option to forego a hysterectomy, there are many alternatives that work with hormonal support and lifestyle changes to relieve and treat heavy bleeding, endometriosis, fibroids and polyps. Current treatment options include:
- medical/hormonal management
- D&C and hysteroscopy
- endometrial ablation
- MRI–guided focused ultrasound (MRgFUS)
- laparoscopy and endometriosis excision
- myomectomy
- uterine artery embolization (UAE)
Success rates of these techniques vary, so it’s important to support whatever method you pursue with the healthiest lifestyle choices you can make. Many women get excellent results with the nutritional guidelines that come with our Hormonal Health Programs, and also use our Nurse–Educators to help them recover from a variety of procedures — including hysterectomy.
Looking ahead
Heavy bleeding or a diagnosis of fibroids can be distressing and scary but it is rarely necessary for a woman to jump right into surgery. Checking out other possibilities may steer you in an entirely different direction, so if possible, take the time to evaluate all options.
Because hysterectomy and fibroids are so common, studies into other treatment options are underway, and new techniques are being developed and researched in many parts of the world. Results so far are mixed, but these less invasive techniques do work for some women.
No scientific, randomized study has been done to fully evaluate these various hysterectomy alternatives, their side effects, risks and benefits. Some observational studies on UAE have been done, comparing outcome satisfaction, failure rates, and cost compared to traditional hysterectomy methods.
Your choices today
For many women hysterectomy is a choice. Exploring the other natural and less invasive alternatives is valid — as is surgery, if it comes to that. It’s also true that some women feel wonderful after their hysterectomies and have no side effects. Whether you opt for a nonsurgical alternative or some version of hysterectomy, consider boosting your nutrition and taking steps to balancing your hormones.
1 Farquhar, C., & Brosens, I. 2006, Mar 22 [Epub ahead of print]. Best Pract. Res. Clin. Obstet. Gynaecol. Medical and surgical management of adenomyosis.
2 Ohanlan, K., et al. 2006, July 7; [Epub ahead of print] Total laparoscopic hysterectomy for uterine pathology: Impact of body mass index on outcomes. Gynecol. Oncol.
3 American College of Obstetricians and Gynecologists Committee on Gynecologic Practice. 2006. ACOG committee opinion. No. 337: Noncontraceptive uses of the levonorgestrel intrauterine system. Obstet. Gynecol., 107 (6), 1479–1482.
4 Society of Interventional Radiology. March 2006. URL: https://www.sirweb.org/refSpec/GR_PDFs/UFE_Grand_Rounds.pdf (accessed 07.27.2006).
Further reading
Society of Interventional Radiology
OB/GYN.net
Relieve your hormonal
imbalance symptoms today
- For perimenopause and menopause symptoms
- Natural and easy-to-take
- Satisfaction always guaranteed