If you’re a woman heading into menopause – or perhaps already there – and you know you have an underactive thyroid, you may be wondering how your low thyroid function might impact this transition. Or, maybe your thyroid function is normal, and you’re simply wondering whether menopause will change this.
 Well, your hunches are right-on that hypothyroidism and menopause can be interrelated, just like the rest of our endocrine (hormonal) system!
Well, your hunches are right-on that hypothyroidism and menopause can be interrelated, just like the rest of our endocrine (hormonal) system!
What is hypothyroidism?
Your thyroid plays a key role in helping you metabolize food, store and use energy, manage your weight and temperature control, think, talk, and sleep. Hypothyroidism is characterized by an underproduction of the hormones needed to support your activity on a daily basis. As a result, you may experience fatigue, poor concentration, cold sensitivity, weight gain, dry skin, hair loss, and general sluggishness.
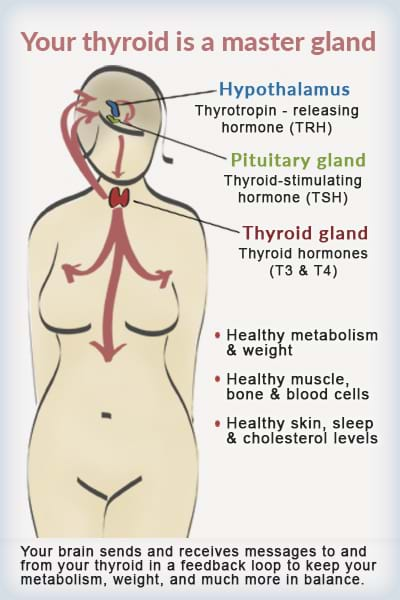
Normally, your brain and thyroid communicate with your body to maintain optimal balance. In a healthy state, the brain produces thyrotropin-releasing hormone (TRH) and thyroid-stimulating hormone (TSH). TSH prompts your thyroid to produce the thyroid hormone T4 (thyroxine), which is then converted in other parts of the body to T3 (triiodothyronine), the form our cells use most effectively. In the case of hypothyroidism, either the thyroid’s ability to make and release T4, or the body’s ability to convert T4 to T3, becomes compromised, often showing up in the form of elevated TSH.
Menopause can “tip the scale” toward hypothyroidism
You may have lived your entire life without realizing you were vulnerable to thyroid imbalance. Ideally, the body can smooth out the major transitions women experience across their life spans. But there are many factors that can trigger thyroid imbalances in women, including menopause and hormonal changes (see chart) stress, and nutrition. Women, in general, are more prone to thyroid disorders than men.
Hypothyroidism is also more common in older women than in younger women. One reason for this is that autoimmunity develops more easily with aging, including autoimmune thyroid disease. This condition — the primary cause of thyroid imbalance in the US — is a situation in which your own cells attack the thyroid gland. Premenopausal levels of estrogen help our immune system to ‘tolerate’ our own cells, and a decline in estrogen makes this less efficient.
Is this menopause or hypothyroidism?
What makes women vulnerable to thyroid imbalances?
- Stress
- Environmental exposures
- Suboptimal nutrition
- Genetics
- Hormonal flux (puberty, birth control pills, pregnancy, menopause, HRT)
In menopause, our bodies naturally produce fewer reproductive hormones because we have less need for them during the second half of our lives. This is normal, and the transition for many women is a smooth one, especially given healthy adrenal glands (more on this below).
But for other women, especially those who have experienced unrelenting stress in the years leading up to menopause, this change of life can bring with it uncomfortable symptoms like low energy, depression, fuzzy thinking, worsening memory, lower sex drive, hair loss, and easier weight gain. If you’ve had low thyroid function, you’re probably already all-too-familiar with these same symptoms! Indeed, many symptoms of hypothyroidism overlap with menopausal symptoms, making them difficult to tease apart. Further complicating matters is the fact that low thyroid function can also exacerbate menopause symptoms.
Our Symptom Screener may help you to get to the bottom of your symptoms. It’s also a good idea to get your thyroid checked. I recommend testing for:
- TSH levels
- thyroid hormone levels
- thyroid antibodies
Elevated antibodies indicate autoimmune thyroiditis, which can lead to overt hypothyroidism down the road if not addressed. A TSH above ~2.5 mIU/L (most labs’ TSH cutoff is 4.5 or 5) suggests that your thyroid is probably underactive.
Hypothyroidism and hormone replacement therapy
Getting tested is especially important for menopausal women who decide to use hormone replacement therapy (HRT). This is because HRT (at least the oral form) can lower bioavailable T4. This means that if you’re already on thyroid treatment, your dose may need to be increased, and if your free T4 levels have been normal, they may drop a bit for the first time.
Thyroid imbalances can increase your risk of:
- Cardiovascular disease
- Atherosclerosis
- Heart attack
- Peripheral vascular disease
- Increased cholesterol
- Cognitive decline
- Bone loss
This happened with a patient of mine. She was newly menopausal and determined to “stay young.” Another doctor had started her on Premarin and Provera, but instead of feeling better, she felt worse. She was experiencing water retention, weight gain, depressed mood, and trouble concentrating. Because she was taking oral HRT and also had rheumatoid arthritis (an autoimmune disease), I checked thyroid levels and thyroid antibodies. Not surprisingly, her TSH was mildly elevated, her free T4 was low, and she had elevated antibodies. I switched her to a more natural and topical form of HRT, and also started her on natural thyroid formula containing both T3 and T4. Over time, her thyroid and adrenal health improved through lifestyle modification, targeted nutrition, and herbs. Her thyroid dosage requirements also dropped over time.
The importance of healthy adrenals in menopause
Sometimes the origins of thyroid imbalance don’t lie within the thyroid gland itself, but rather in other parts of the endocrine system. Excessive cortisol (an adrenal hormone) from severe stress can blunt the TSH response to TRH or T4. Too much or too little cortisol can also impair the conversion of T4 to T3. With poor conversion, it’s even possible to experience symptoms of both high (T4) and low (T3) thyroid simultaneously. Chronic stress over time can fatigue our adrenals, making it difficult for them to keep pumping out cortisol on demand.
On top of its effects on thyroid, chronic stress can foster a more difficult menopausal transition. As ovarian function declines, our adrenal glands continue to produce hormones including androgens that convert to estrogens. One of these androgens is DHEA, an important contributor to libido, sense of well-being, bone health, and proper immune function. If our adrenal glands are tuckered out by the time we enter menopause, all of these hormones can plummet.
Supporting your thyroid naturally
Starting with a gentle, natural approach may help to restore normal function and decrease any thyroid symptoms that overlap with menopause symptoms. Depending on the degree of imbalance, you may require a prescription for thyroid hormone. Even so, the following simple measures can help to support your thyroid naturally:
Get checked. Regular screening and wellness exams are particularly important as you move into menopause. If you have a personal or family history of thyroid conditions or any autoimmune disease, be sure to inform your healthcare provider and ask for thorough testing.
Nourish yourself. Your body needs a wide range of nutrients every day to manufacture and metabolize thyroid hormones. Be sure to eat food that include vitamin A, vitamin D, zinc, iodine and selenium. It’s also a good idea to get EPA and DHA (e.g., fish oils). Selenium and vitamin D are especially helpful in protecting against thyroid autoimmunity.
Healing herbs from Mother Earth. Medicinal herbs can not only help women in peri-menopause or post-menopause to recalibrate the ratios between estrogen, progesterone, and testosterone, but can support healthy thyroid metabolism as well. I recommend bacopa, hops, and sage, which are all found in our T-Balance Plus, to support healthy metabolism within the thyroid gland and throughout the body.
Manage the level of stress in your daily life. Chronic stress has powerful, detrimental effects on your endocrine system. You may not be able to eliminate all stressors in your life, but you can take measures to minimize the impact of stress through moderate exercise, meditation, or other mindful practices. Learning to say “no”, taking time out each day to quiet your nerves, ensuring a good night’s sleep, and minimizing stimulants can all work to keep your adrenals — and, by extension, your entire endocrine system — healthy.
Look for a connection
The transition into menopause, though normal and often smooth, can be bumpy for some of us. Chronic stress, environmental toxins, and genetic predisposition can all tip the scale toward the development of hypothyroidism in menopause, producing symptoms that are remarkably similar to menopausal symptoms. By paying careful attention to your symptoms, you can more quickly make the connection, get evaluated, and start supporting your health in ways that help you to feel your best in your later years.
Badawy A, State O, Sherief S. Can thyroid dysfunction explicate severe menopausal symptoms? J Obstet Gynaecol. 2007 Jul;27(5):503-505.
Schindler AE. Thyroid function and postmenopause. Gynecol Endocrinol. 2003 Feb;17(1):79-85.
Mazer NA. Interaction of estrogen therapy and thyroid hormone replacement in postmenopausal women. Thyroid. 2004;14 Suppl 1:S27-34.
Hak AE, Pols HA, Visser TJ, et al. Subclinical hypothyroidism is an independent risk factor for atherosclerosis and myocardial infarction in elderly women: the Rotterdam Study. Ann Intern Med. 2000 Feb 15;132(4):270-8.
Rodondi N, den Elzen WP, Bauer DC, et al. Subclinical hypothyroidism and the risk of coronary heart disease and mortality. JAMA. 2010 Sep 22;304(12):1365-74.
Pizzorno L. Clinical Approaches to Hormonal and Neuroendocrine Imbalances. In: Jones DS, ed. Textbook of Functional Medicine. Gig Harbor, WA: The Institute for Functional Medicine; 2010:644-650.
Badawy A, State O, Sherief S. Can thyroid dysfunction explicate severe menopausal symptoms? J Obstet Gynaecol. 2007 Jul;27(5):503-505.











